WellCare Health Plans Inc
Latest WellCare Health Plans Inc News and Updates
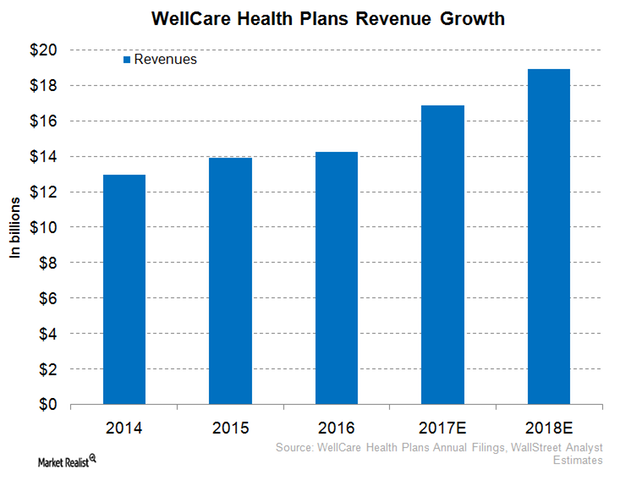
WellCare Health Plans Expects Robust Revenue Performance in 2017
In 1Q17, WellCare Health Plans (WCG) reported revenues of ~$3.9 billion, which totals year-over-year growth of around 11.7%.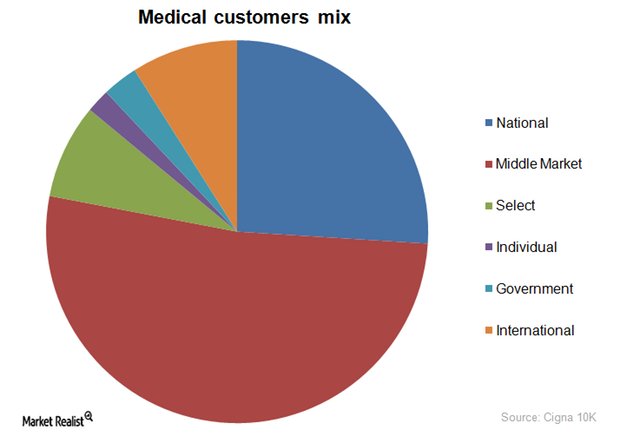
Cigna’s Customer Segments a Healthy Mix
Customer segments The players in the private health insurance industry (IYH) aim for a favorable enrollment mix to reduce taxes and other liabilities while at the same time generating sustainable profits. Accordingly, managed care organizations such as Humana (HUM), Aetna (AET), Anthem, Cigna (CI), and WellCare Health Plans (WCG) are increasingly focusing on government-sponsored and international enrollments to balance […]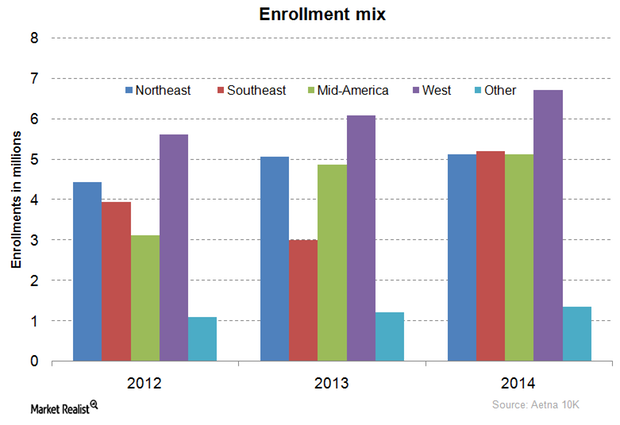
How Is Aetna’s Membership Distributed Across Its Key Markets?
Aetna’s membership is mainly concentrated in the western US, followed by the Southeast, the Northeast, the Mid-US, and finally consolidated international enrollments.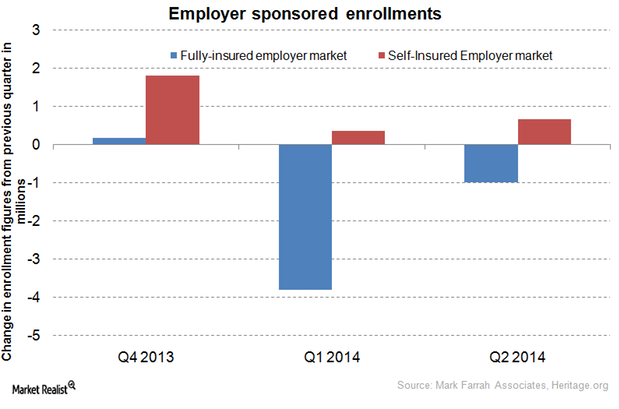
Shift to self-insurance plans affects health insurance stocks
As hospital utilization remains low, more employers are exploring the option of self-insurance to reduce their employee benefit costs.
